There’s a Massive Gap in Care
35%+
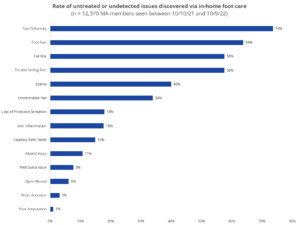
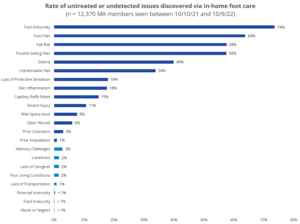
Seniors have a hard time caring for their feet… 35%+ can no longer reach or see their feet
1000
+
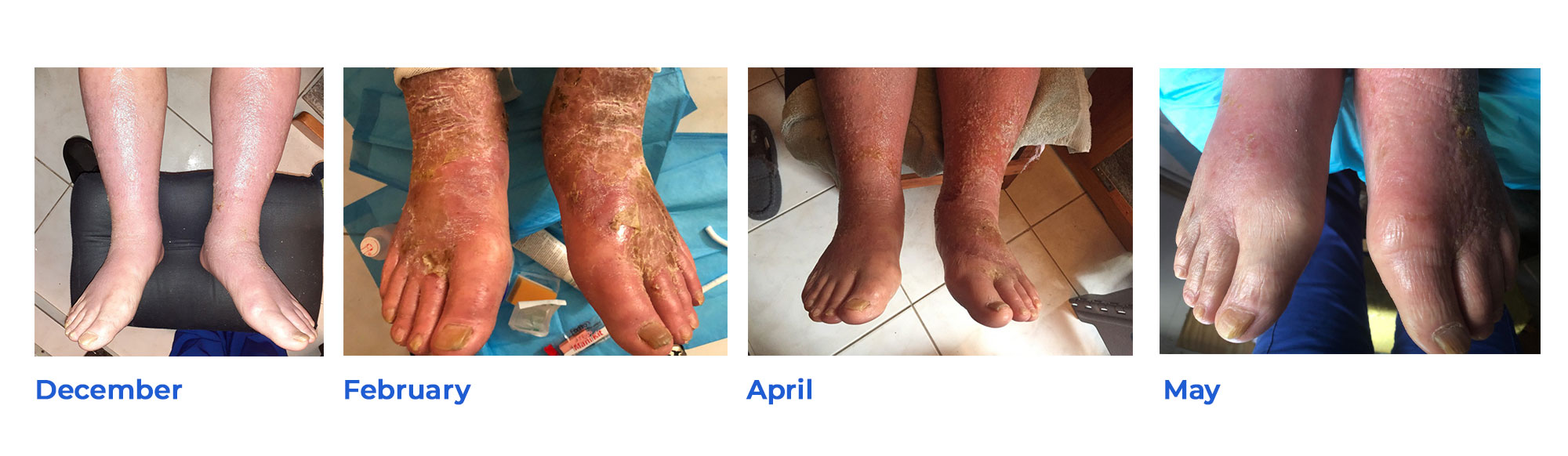
As we age, worsening chronic conditions like diabetes and vascular disease drive 1M+ U.S. foot ulcers and amputations every year
1
Billion Dollars
For diabetes alone, foot complications drive 1 out of 3 dollars of medical spend – a whopping $38B
85%
85% of these foot complications are preventable, yet still happen

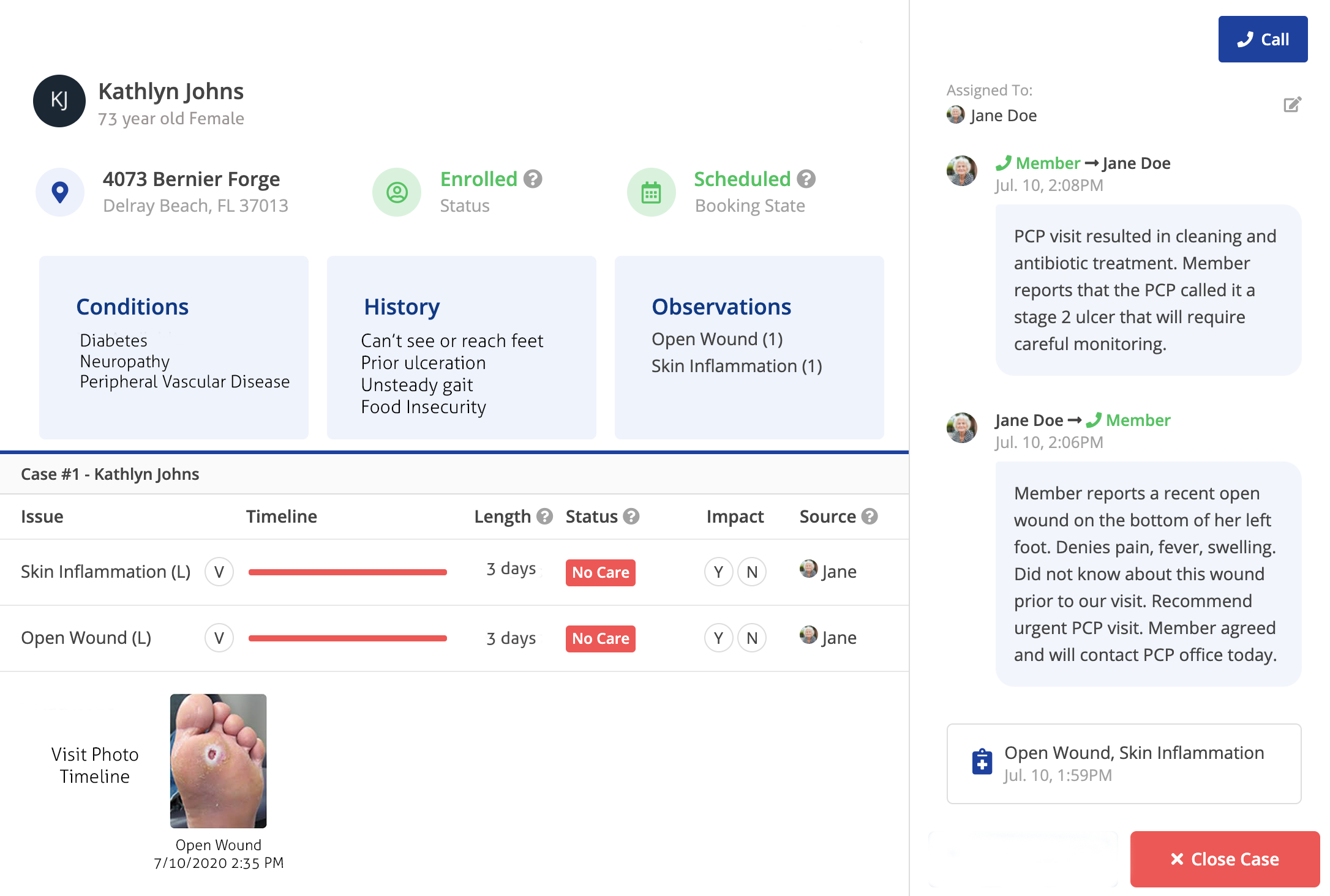
Belle is the in-home ambassador for health plans
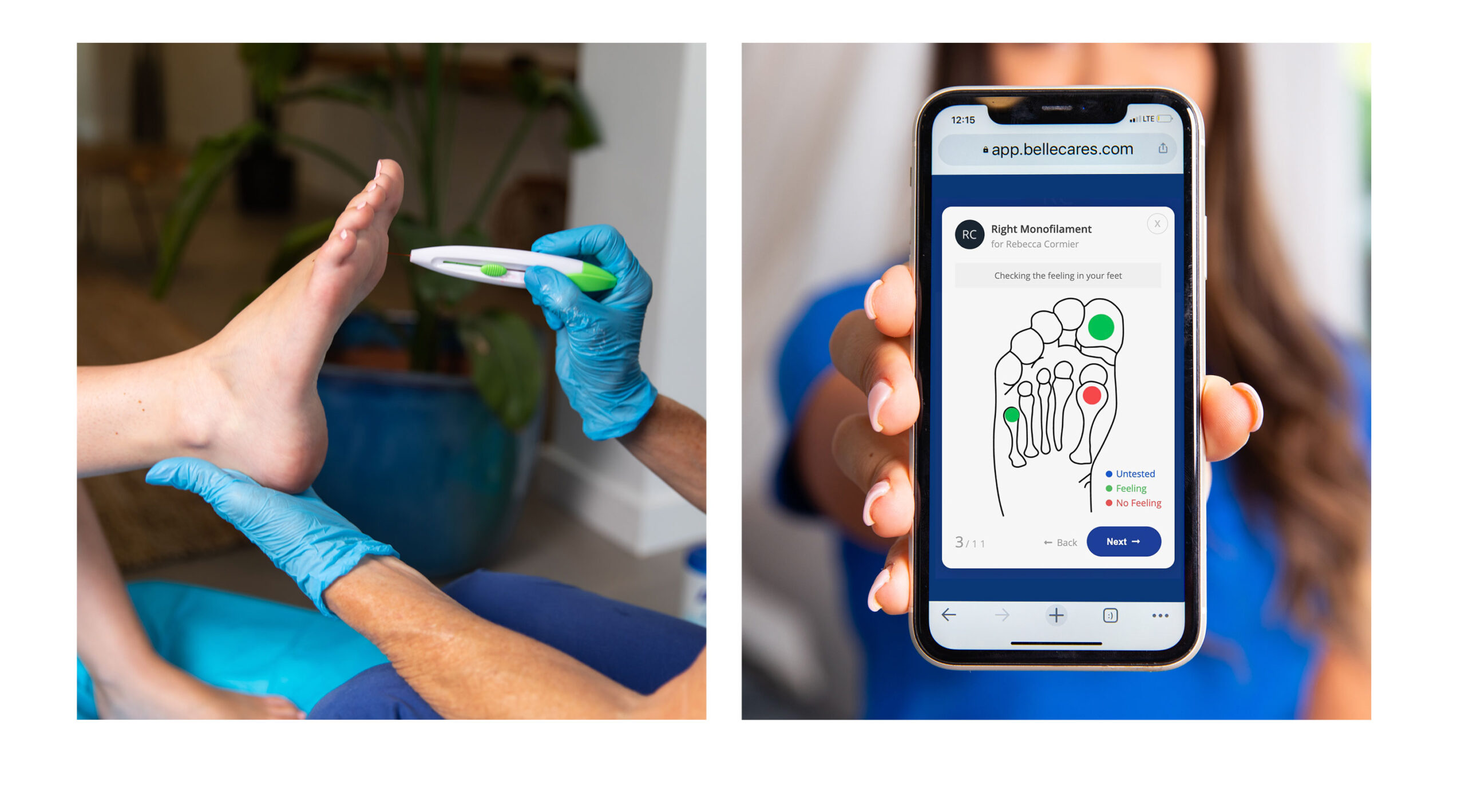
To address this gap in care, Belle provides protocol-driven, preventive foot care. We partner with health plans to develop deep-rooted relationships that drive joy, trust and loyalty among beneficiaries.
With in-home visibility, Belle delivers a holistic picture of a member’s health. Our member experience is unprecedented. Over 98% of our members book another visit.
Our standing monthly visits build long lasting relationships with members and their households. We often find ourselves at the center of it all, connecting the right people together for a common purpose.
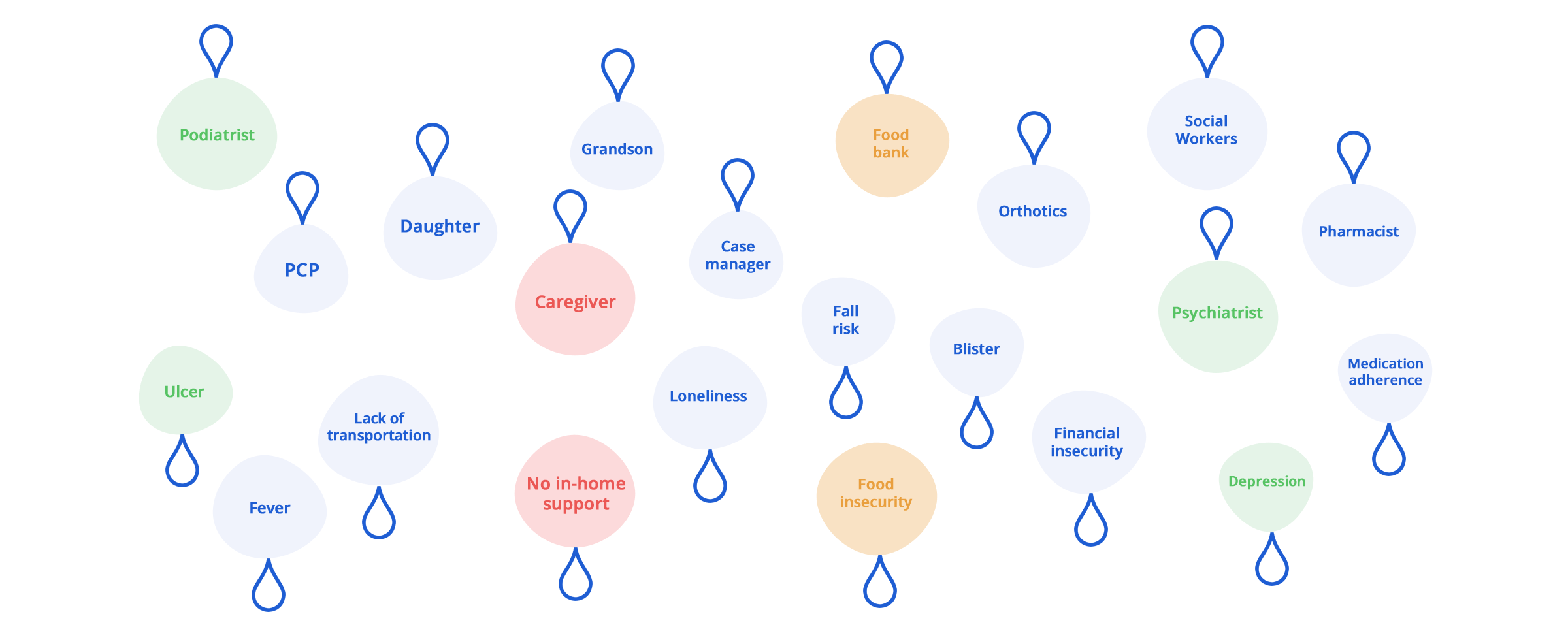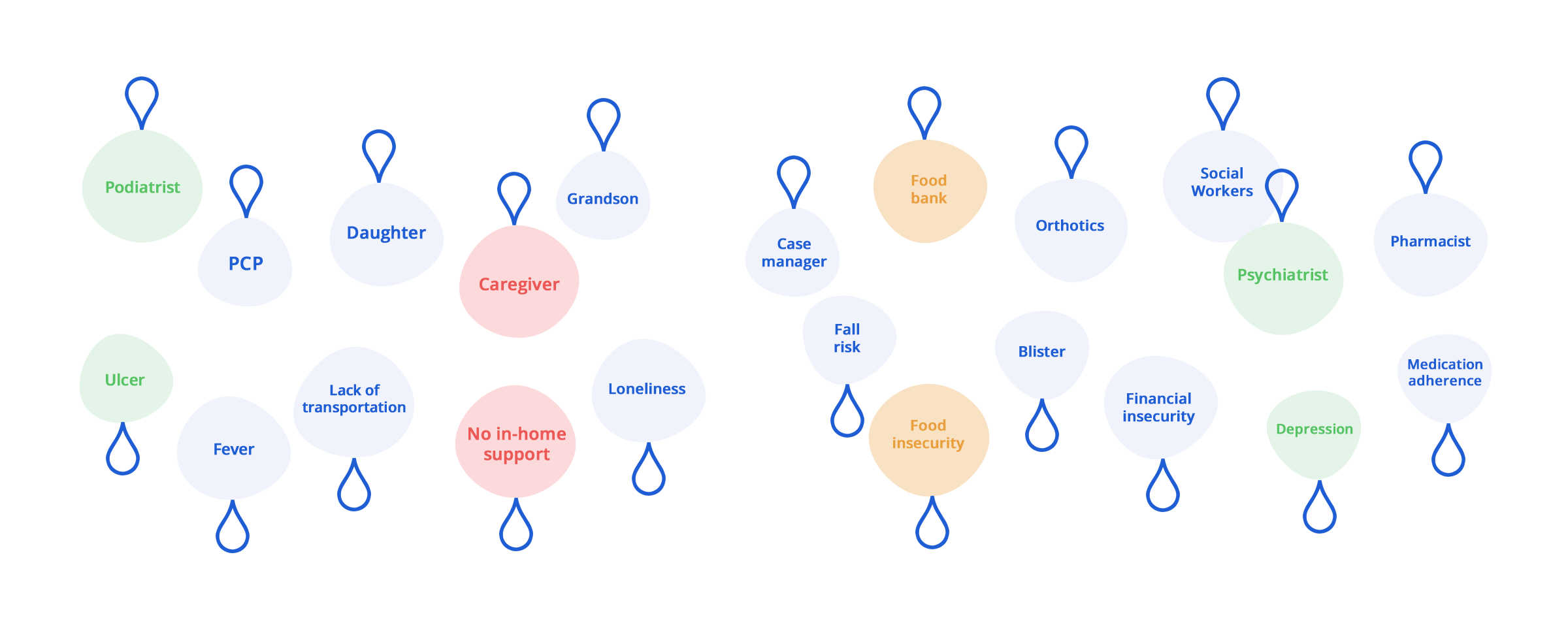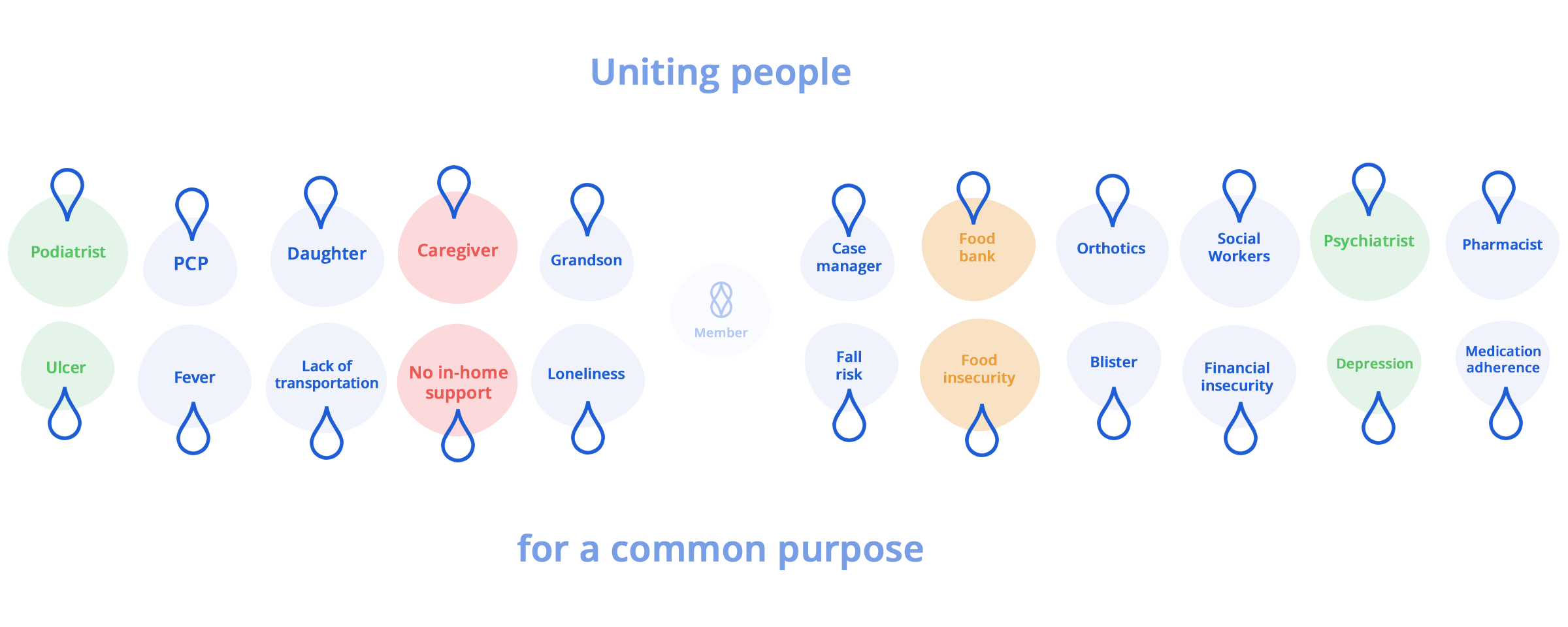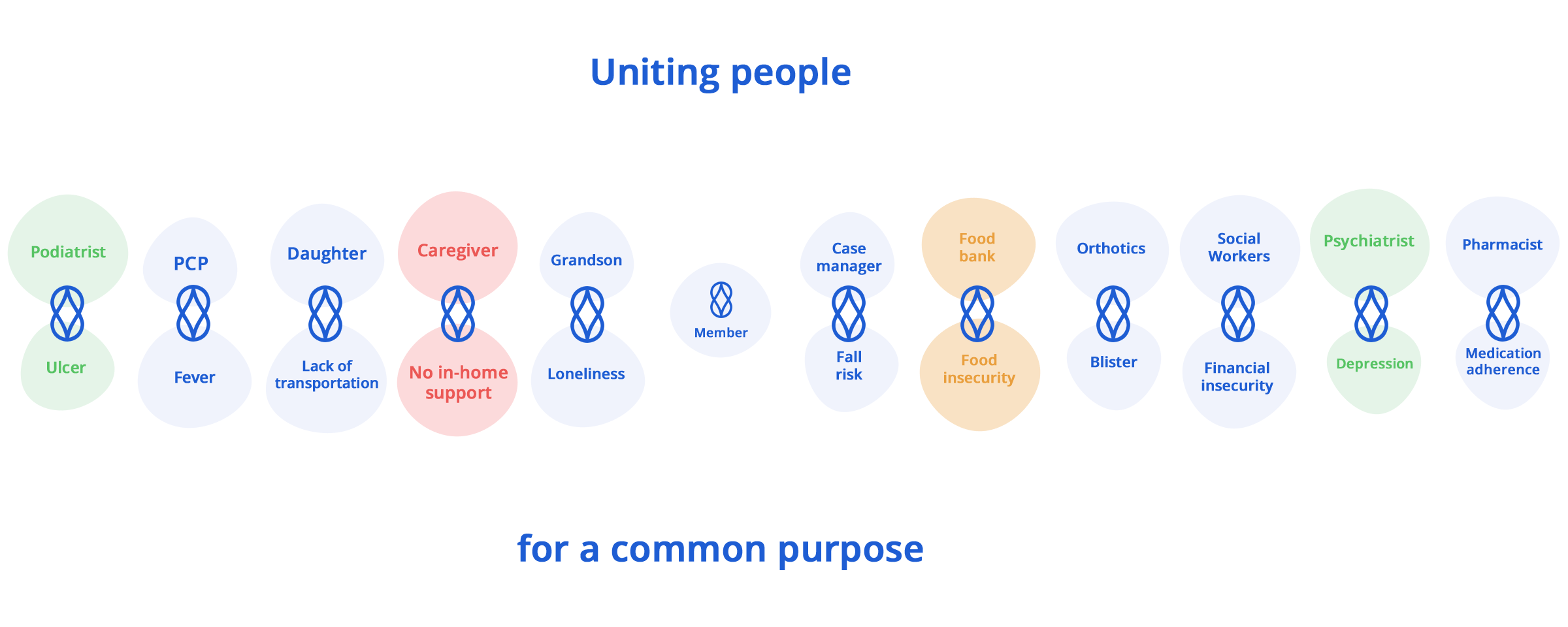
Our service is not only closely tied to the member’s community, but also other in-network providers and case managers. All to facilitate team-based interventions and resources when needed. Our proprietary technology is designed for this purpose, giving our techs and clinical team the tools they need to make each home visit count.
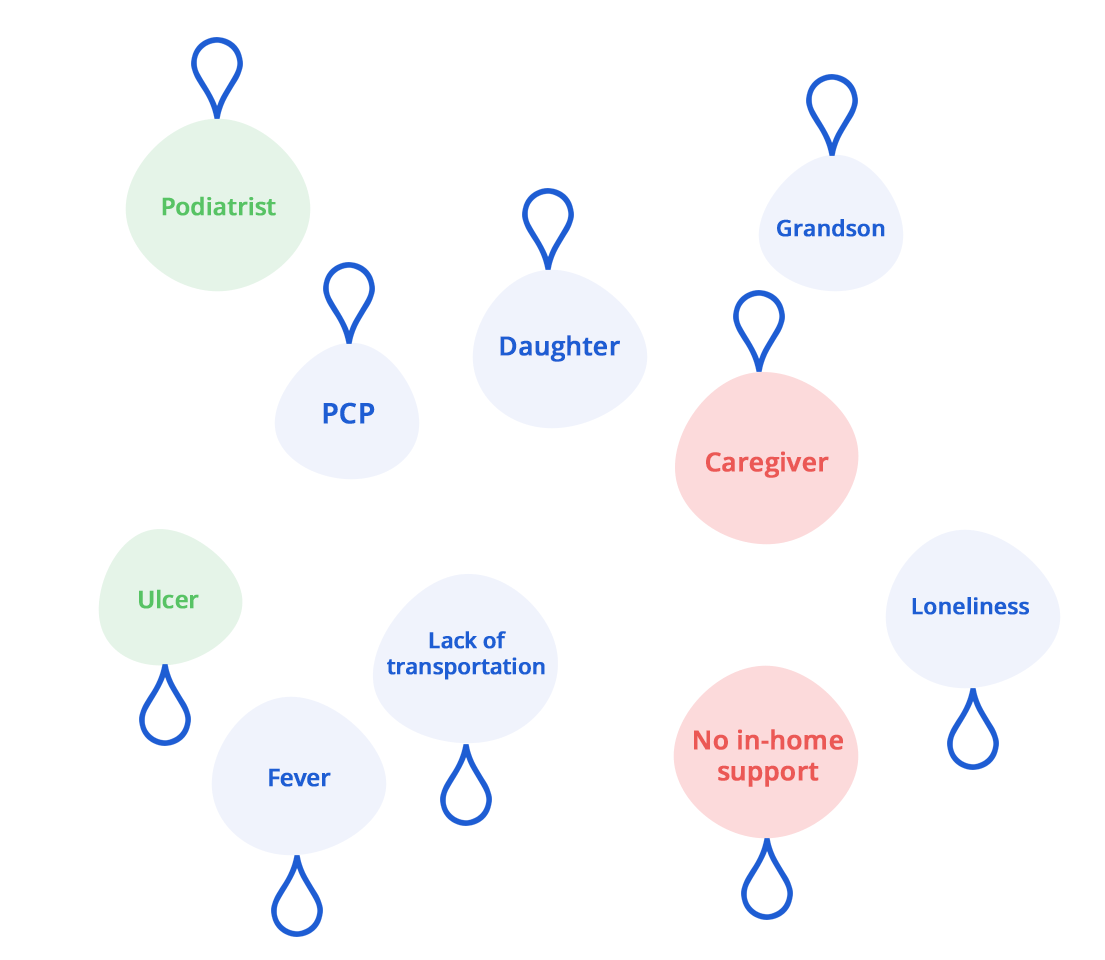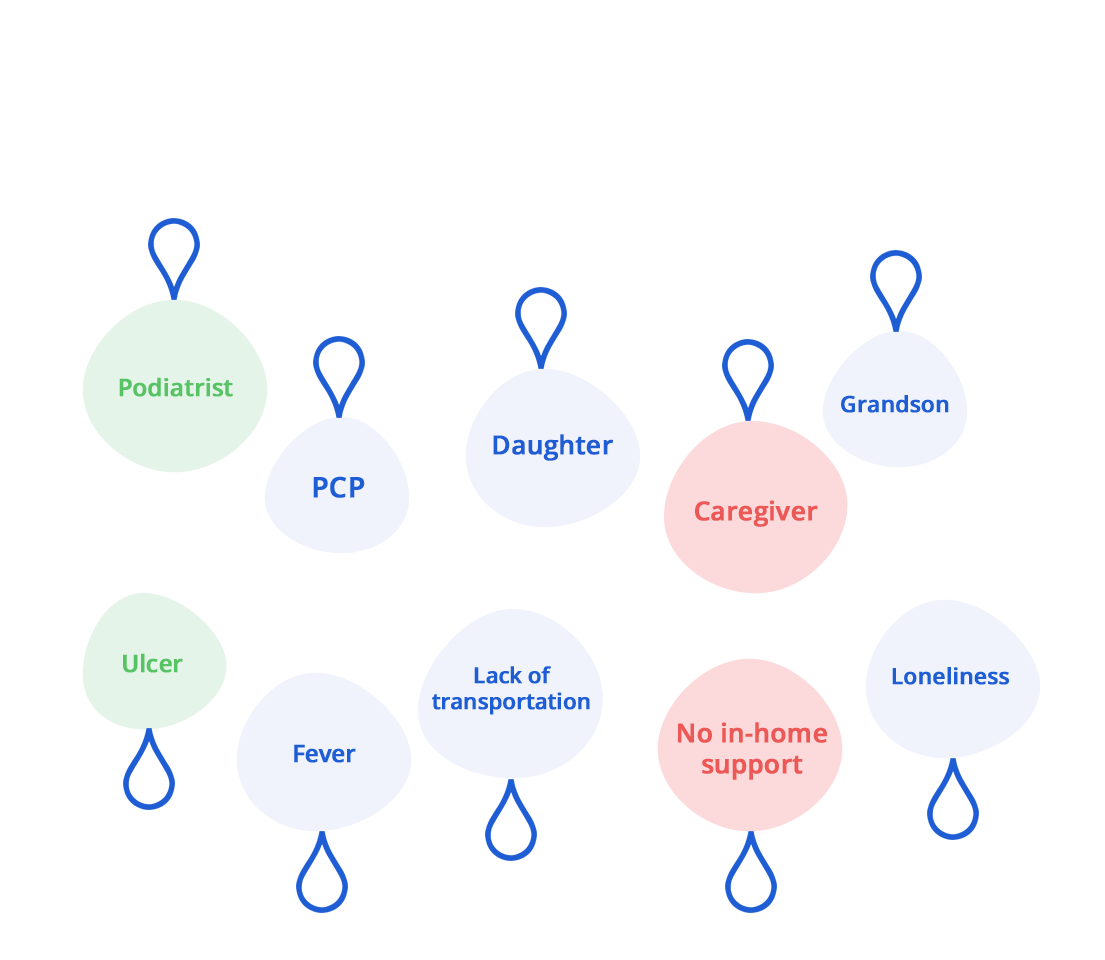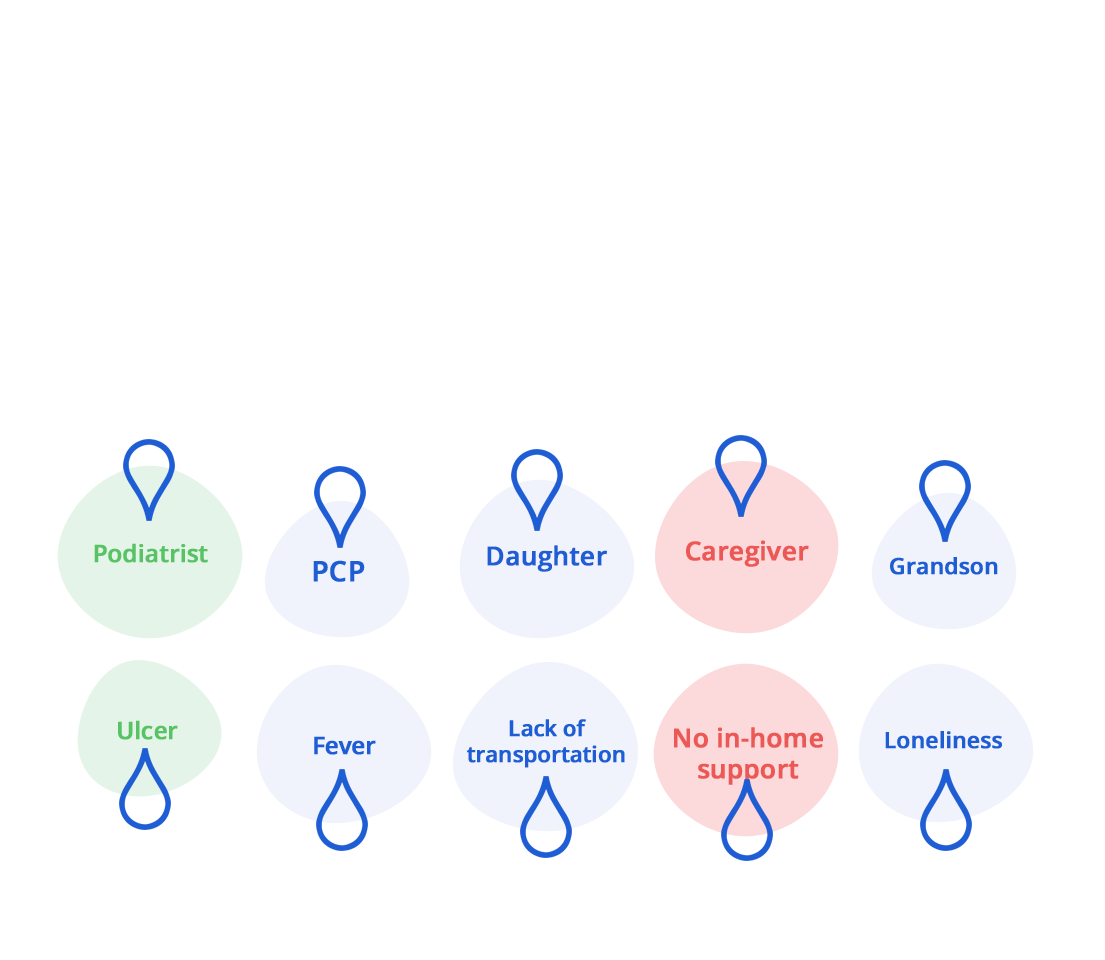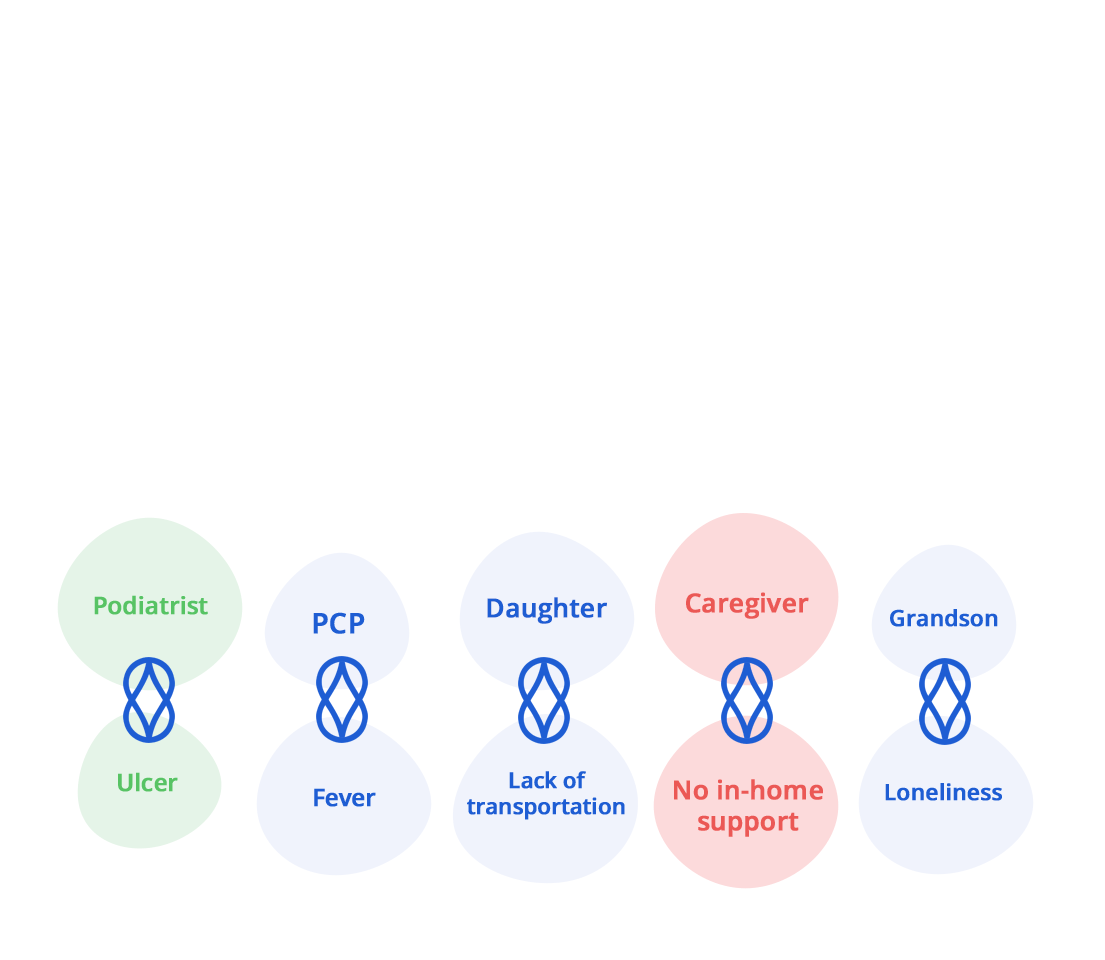

Our service is not only closely tied to the member’s community, but also other in-network providers and case managers. All to facilitate team-based interventions and resources when needed. Our proprietary technology is designed for this purpose, giving our techs and clinical team the tools they need to make each home visit count.

We Provide 4x+ ROI
Member Loyalty
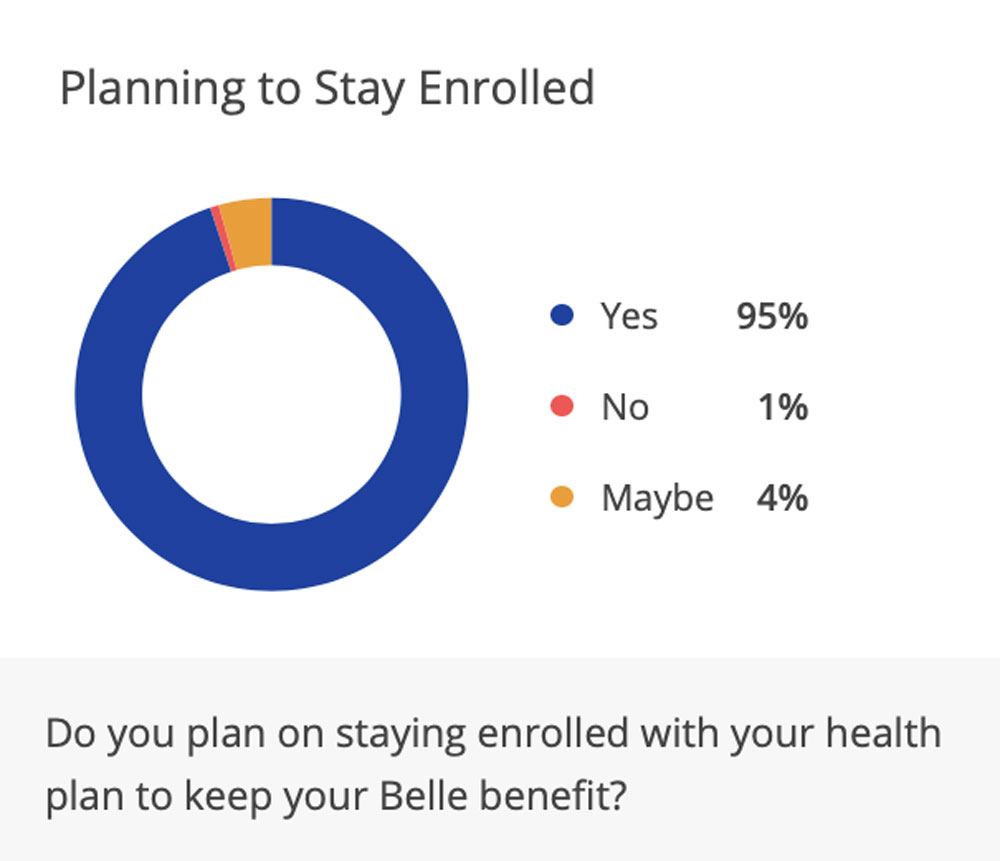
The Belle visit is a time when a member can sit back, relax and enjoy a conversation with a friend. The joy we create translates into health plan loyalty. We reduce disenrollment by 40%+ for those enrolled.
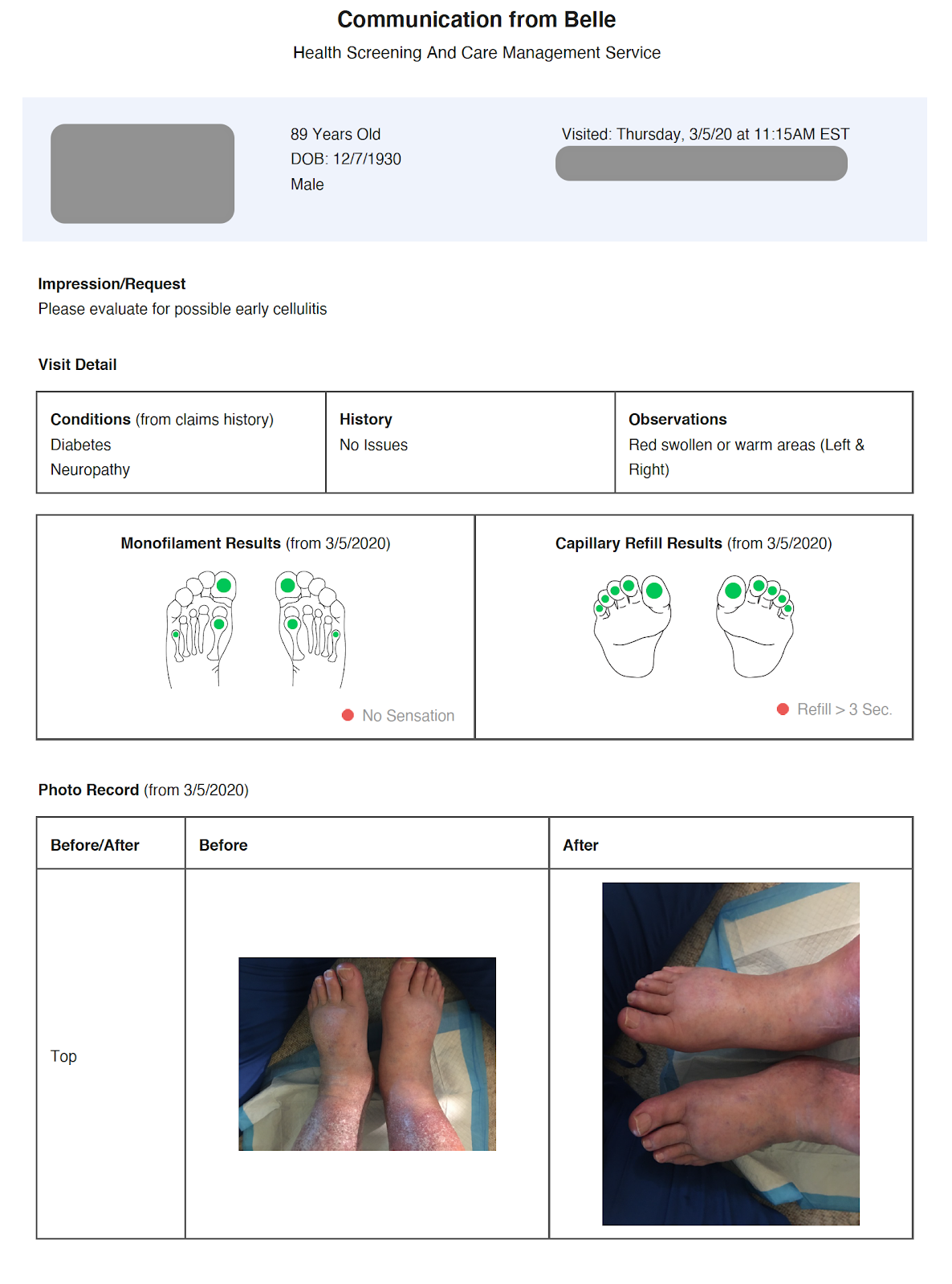
Longitudinal Data
We track physical, mental and emotional health issues over time.
Case Management Partnership
We work with our health plan partners to create a powerful flow of critical, actionable insights that empowers the healthcare ecosystem.
Screening
Our regular clinical tests and interventions consistently find new diagnosed conditions, bringing care to members faster and improving coding processes.
Member Insights
We offer unprecedented intelligence through our service and technology. Our insights range from HEDIS and Star Rating indicators to SDoH and accurate contact information.
Influencing Behavior
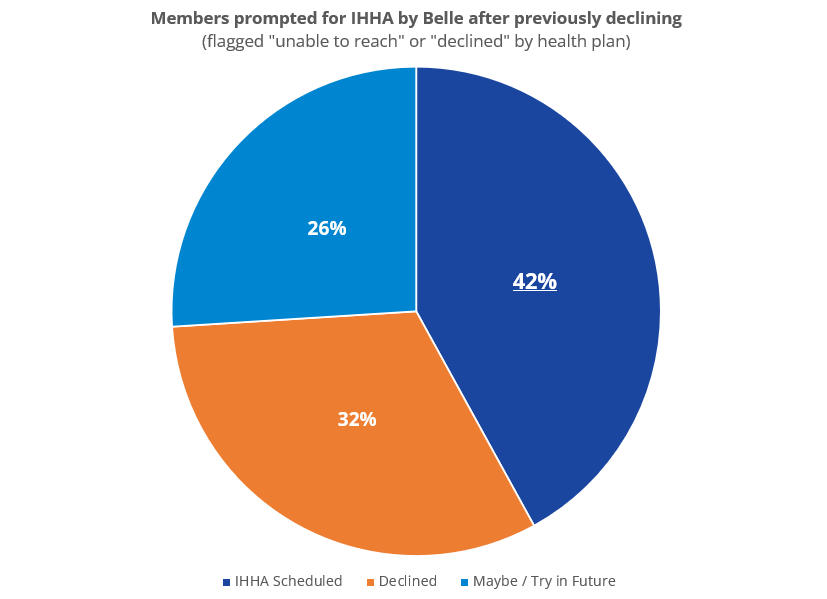
A free pedicure that closes a practical gap in care gets us invited into homes of thousands of members who are typically skeptical or disengaged
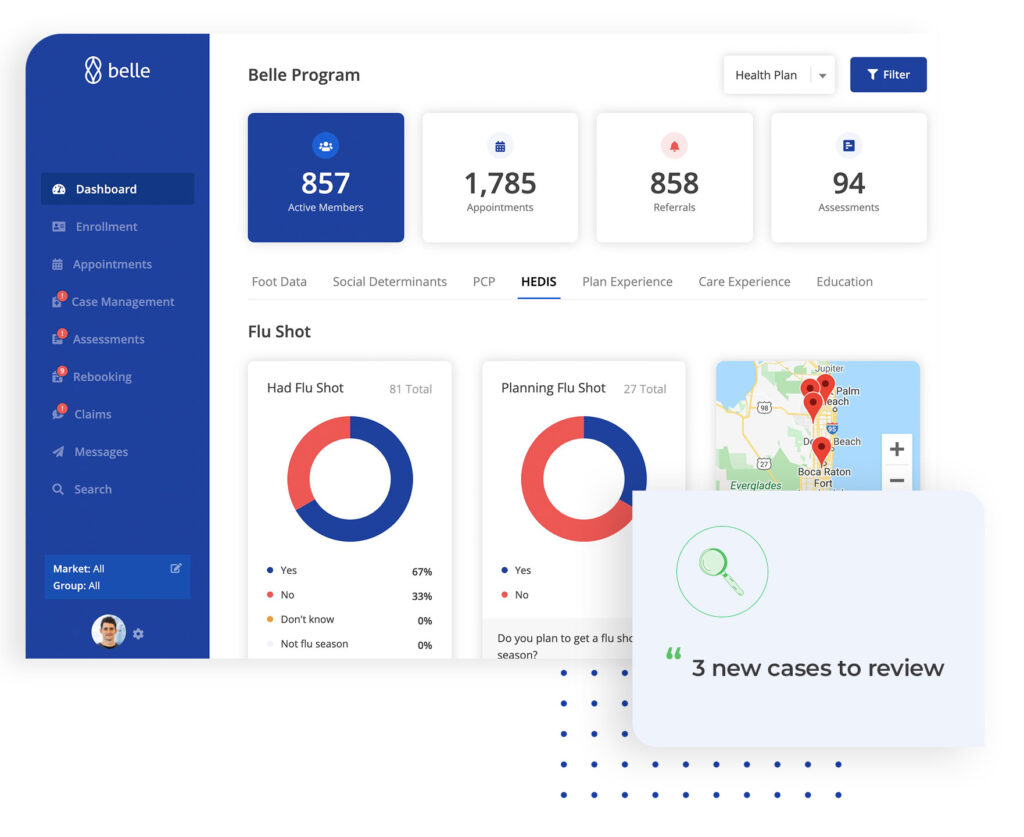
Expanding Nationally
Launching the Belle care management program is easy. Belle typically contracts with health plans as an in network provider, but can also be offered as a supplemental benefit. New regions can be up and running in 60 days.
Contact us to learn how it works.

“I learned to be much more aware of taking care of my feet. I was walking around barefoot all the time.”
“There really isn’t any other kind of service like Belle!”
“It was really pleasant to have someone take care of my feet…I’m really glad Humana jumped on the bandwagon…I’m telling all my friends about it!”
“[Belle] really is such a blessing for me. It is so appreciated.”
“I may be moving soon and I wanna know what resources I’m gonna have, because now, already, Belle is a prime resource for me.”